|
Gynecomastia correction is a commonly carried out procedure among men.
The aim of the surgery is an improved contour of the chest. This is accomplished with the help of minimal incisions such that patients do not have an operated look. Most of the patients undergoing correction have liposuction for removal of the fat surrounding the gland and in the lower part of the axilla (armpits). The incision is placed in the areola (pigmented skin around the nipple) for removal of the gland. The areolar incision usually settles very well and has a high patient satisfaction. We sometimes place small tubes (drains) to remove any fluids from the operated site. This is usually removed on the next day. Many of our patients do not have a drain. Most of the cases of gynecomastia correction are performed under general anesthesia. We reserve treatment under local anesthesia for cases with minimal gynecomastia in slim individuals. Patients are retained overnight after the procedure. Dressings are removed and operated area is inspected on the day after the surgery. Patients are instructed to wear pressure garment continuously for a month following the surgery. They are usually discharged home after an overnight stay. Due to liposuction and accompanying infiltration of the operated sites with local anesthetic most patients are comfortable on oral pain medications. At home, patients can move about and carry light activities. We review our patients back in the clinic 2 to 3 days after the procedure. The dressings are removed and skin adhesive tapes are used to secure the suture line. Patients can shower with the skin adhesive tapes. We review the patients after one week for removal of sutures after one week. Skin adhesive tapes are reapplied for 2 more weeks. Most patients usually return to work within a week. Heavy exertion such as weight lifting is restricted until one month following the procedure. A normal recovery can involve the following,
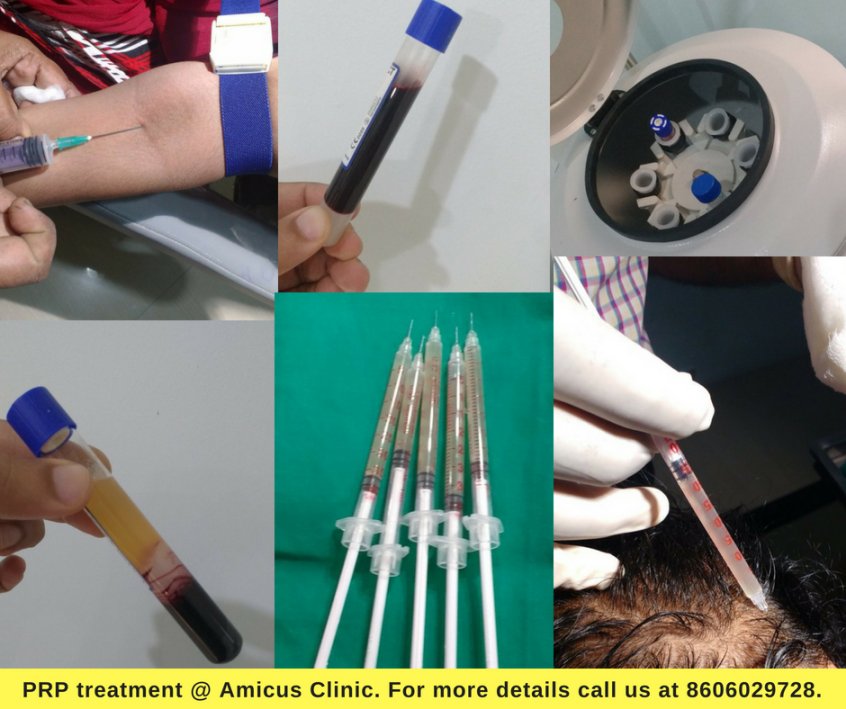
In most patients, gynecomastia correction is associated with a boost in self-confidence. Learn more about gynecomastia here. For more information about PRP | Platelet-rich plasma, click here
Get in touch with us at, 8606029728. An axillary breast is a common condition that affects women. It presents as a swelling over the axilla (armpits). The severity may vary from a mild bulge to a loose baggy fold. Those affected by this condition often view this as unsightly and avoid wearing clothes which reveal this condition.
This axillary swelling is usually an extension of the breast tissue from the outer and upper quadrant. This tissue is also prone to the same changes which occur in the rest of the breast. There may be accompanying pain and discomfort in certain phases of the menstrual cycle. The axillary breast is usually removed as a daycare procedure. Patients are usually discharged home after a brief period of rest following the procedure. Liposuction and open removal (axilla-plasty) are two techniques that are combined to treat this condition. Liposuction is used to remove fat from the edges of the wound. It helps in the removal of the fat with short incisions. Open removal of the breast tissue has the advantages in allowing better preservation of the nerves which travel through this space. It also helps get rid of the relatively non-retractile axillary skin. The removal of the excess skin gives a better contour to the axilla (armpit). Wounds are approximated with sutures and dressings are applied. Drains are sometimes placed to avoid any collection from occurring at the operated site. Patients are followed up as outpatients and sutures are removed at one week. The postoperative swelling usually resolves over the next few weeks. Patients are usually able to resume work after a few days. There are no restrictions on any activity after a month following the procedure. Treatment of the axillary breast gives a better contour to the axilla (armpit). Liposuction and open removal when combined help women achieve better contours with short incisions. After the procedure patients usually feel more confident about their appearance. You can learn more about female breast reduction here. The hymen is a diaphragm-like structure located at the external opening of the vagina. The aperture(s) in the hymen helps in the drainage of the menstrual blood. The hymen varies in appearance. Some individuals may have multiple apertures instead of a single aperture in the center. It can be either a thin or a relatively thick structure.
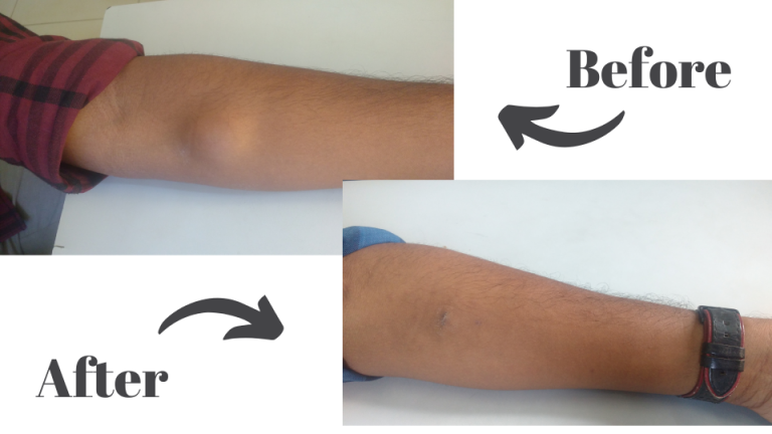
The hymen gets disrupted following sexual intercourse. Following disruption, the hymenal remnants at the external vaginal opening are known as hymenal carunculae. The hymen can also get injured following clinical examination, strenuous physical exercise or disease. hence its appearance is not a definitive indicator of the virginity of a woman or a girl. The presence of an intact hymen in a bride is considered very important in some cultures. This probably arises from a correlation between an intact hymen and virginity. It is possible to repair a laceration of the hymen. This procedure is also known as hymenoplasty. Some also know this cosmetic surgery as 'revirginization'. It is a small procedure which does not require an overnight stay in the hospital. We usually perform this procedure under general anesthesia. The remnants of the hymen are carefully brought together in layers using fine absorbable stitches. Follow up is done after a few days as an outpatient. Patients should avoid strenuous activity for a few weeks following the procedure. The labial folds should not be stretched apart for a month following hymenoplasty. We recommend at least six weeks for the tissues to heal. There are no restrictions on any activity after this period. Hymenoplasty is a relatively new technique among other female genital cosmetic procedures. It may help some individuals cope with the stress arising as a result of the cultural taboos of our society. Lipomas are small soft swellings commonly found beneath the skin. Lipomas are usually painless. In most cases, they are accidentally detected while touching the area. In some individuals, they can be large and obvious from a distance. Some of us tend to get multiple lipoma over the body and face. This condition is known as lipomatosis. This may run in certain families. Lipomas are removed either to ascertain the diagnosis or because they are considered unsightly. Lipoma removal is usually an outpatient procedure. Patients can go back home after the surgery.
The traditional technique of removal of a lipoma is with open surgery. An incision placed on the skin is used to dissect the lipoma away from the surrounding tissues. The disadvantage of this technique is the resulting lengthy scar. There is a newer technique which can minimize the length of the scars. This is achieved by means of liposuction. During liposuction, the fat in the lipoma is aspirated with a small tube (cannula) attached to a suction producing device. The tiny cannula is inserted with the help of a small incision. The residual lipoma which remains after liposuction can be removed with the help of a small incision. This technique has significant cosmetic benefits because it leads to a short scar. Thus all scar-related consequences such as hypertrophy, color and texture changes of the overlying skin are minimized. Patients are later reviewed in the clinic. It is usual to have some induration at the operated site. This gradually subsides over the next few weeks. The recovery following this procedure is similar if not faster when compared to the traditional technique for removal of lipomas. Liposuction for the removal of lipoma is a good option for those who want to get it removed with the help of very small incisions. It is especially recommended for individuals with multiple lipoma as the resulting length of the scars are less compared to the traditional open technique. For more information about liposuction, click here. For more information about fat grating, click here. Gynecomastia correction is commonly performed for improvement in the aesthetics. It is done as an outpatient or short stay procedure. Which means that patients do not have to spend a long time at the hospital.
Anesthesia: Depending on the severity of gynecomastia and patient preferences, the corrective surgery is carried out under local anesthesia or general anesthesia. In case of small enlargements carried out under local anesthesia patients are sent home the same day. In case of cases treated with general anesthesia, we opt to retain the patient overnight at the hospital. Returning home: Patients can go home the next day after the change of dressing. Patients are usually comfortable after the surgery and most report only minor discomfort and do not require multiple analgesics. Patients can shower next day onwards and are advised to apply a small pad over the suture line. Pressure garments have to be worn constantly for a month. Follow-up: We see patients in our outpatient set up after a few days to check on the healing. During this visit, most of the swelling has started to subside. Some of our patients resume light work after a few days. Sutures (stitches) placed on the areola (pigmented skin around the nipples) are removed at one week. Resuming work and exercise: After a week light exercise like running and walking can be resumed. We see our patients again at the end of a month. By this time, the improved contours of the chest are well made out. After a month there are no restrictions on any activity. We ask for a review at three months and one year after surgery. Most of the patients have an uneventful recovery. Some patients may get prolonged swelling due to postoperative collections. These are usually treated conservatively and settle after a period of time. The collection usually does not make any difference in the final outcome of the procedure. Gynecomastia surgery is associated with a high satisfaction rate and patients report an increase in self-confidence after the procedure. For more information about gynecomastia, click here Male breast enlargement or gynecomastia can be treated effectively with liposuction and direct removal of the gland. And a significant number of such patients can be treated under local anesthesia. With improvements in anesthesia techniques, it is possible to have a near pain free experience. There are certain advantages in undergoing the procedure under local anesthesia. These include:
Some types of gynecomastia are particularly suitable for treatment under local anesthesia. These include:
There are certain disadvantages when doing liposuction and excision under local anesthesia when compared to general anesthesia. Perhaps the most important would be the longer duration of the procedure. Local anesthesia should be allowed to act for a sufficient duration before liposuction is begun. Similarly, it is common to again inject the anesthetic solution and wait before resuming the procedure. The procedure takes longer to complete under local anesthesia. Individuals who are afraid of needles and do not want to be awake during the surgery may not be right candidates for the procedure. To summarize, local anesthesia is a good option if you are adequately motivated and have one of the milder forms of gynecomastia. The advantages include faster recovery and improved safety profile of the procedure. Revision rhinoplasty is a secondary correction of a previously operated nose. It may be carried out for improvement in appearance and breathing (function). A significant number of patients who have undergone rhinoplasty present themselves for revision surgery. According to some reports, this is as high as twenty percent. Why do undergo a secondary rhinoplasty? The dissatisfaction with appearance could be as a result of unrealized expectations or due to the presence of a new deformity. It could be an unexpected result due to scarring associated with the previous surgery. A rhinoplasty is associated with swelling which can last approximately one year. The final shape of the nose is not apparent up to one year following a rhinoplasty. Because of this, it is prudent to wait for at least one year before carrying out a secondary correction. Who is a good candidate for secondary rhinoplasty? A good candidate should have realistic expectations about what can be achieved following a secondary correction. Depending on the existing anatomy there is usually a limit to the amount of improvement that can be achieved with corrective surgery. Also, patients should be in good health. Smokers have significantly higher complications associated with healing when compared to nonsmokers. When is a secondary rhinoplasty performed? Secondary correction is done after allowing sufficient time for the tissues to settle. This usually takes around one year after the first surgery. In the case of corrections undertaken after a second or third surgery, we wait for more than eighteen months. How is revision rhinoplasty different from the primary rhinoplasty? Revision rhinoplasty involves manipulation of tissues which have been altered during a previous surgery. There will be scars as a result of the previous surgery. In many cases, some of these scars would be excised and in others, the scars may be left behind or used as a filler material. Additional support to the nose may be obtained by the use of cartilage grafts from donor sites such as ear or ribs. It is likely that cartilage donor sites within the nose may be exhausted during the primary rhinoplasty. In general, a secondary correction is more difficult and time-consuming when compared to primary correction. How is the recovery following revision rhinoplasty? The recovery following revision rhinoplasty is similar to that of a primary rhinoplasty. A nasal pack may be used for one or two days. Dressings are usually removed after two days. A splint is used in case the bones have been manipulated. Sutures come off within a week. Patients are usually able to resume light work after a week. Most of the swelling disappears within a month. The nose settles into a final shape by approximately one year following surgery. What are the benefits of undergoing a secondary rhinoplasty? An improvement in appearance and function is associated with improvement in self-esteem and confidence. A positive outcome following rhinoplasty is a very rewarding experience for both the patient and the treating surgeon. For more information on rhinoplasty, click here.
Filler injections are most commonly used in cosmetic medicine to treat wrinkles and plump up lips. They are very popular because of the minimal downtime and reliable results.
Our skin becomes thinner as we age. This leads to wrinkles and creases. Loss of volume is also seen in the fatty layer under the skin. This causes sagging of the various youthful highlights of the face. Apparent lengthening of the lower eyelids, the descent of the malar (cheek) mounds and appearance of jowls and prominent folds between the nose and cheek are some of the changes as a result of volume depletion of these deeper layers. Fillers can counteract these changes by providing volume to the skin and the fatty layer below it. Various substances are employed as fillers. For example, hyaluronic acid, collagen, and hydroxyapatite based fillers. They differ in their indications, risks, and duration of action. Hyaluronic acid fillers are perhaps the most commonly employed fillers. Hyaluronic acid is a naturally occurring substance found in the body. Hence they are not associated with allergy following injections. Hyaluronic acid in addition to supporting the tissues also draws in water. This property also contributes to the volume enhancement. This, in turn, leads to a better appearance due to improvement in proportions of the treated areas. Uses of filler injections They are most commonly used for:
Duration of action of hyaluronic acid fillers Hyaluronic acid is metabolized in the body by hyaluronidase enzyme. The duration of action is approximately 8 to 12 months. It is possible to reverse the effect of a filler injection by injection hyaluronidase. Common side effects of hyaluronic acid fillers The most commonly include side effects include swelling, bruising and lumps. These are mostly temporary and last a few days. Cold compresses help in the resolution of these symptoms if they occur. Tyndall effect is a bluish discoloration as a result of superficial injection of the filler in areas with thin skin. Visual disturbances and vascular compromise are very rare complications seen with filler injections. Contraindications for filler injections The following increases the risk of adverse events and constitute contraindications for filler injections:
How does one get a filler injection? A consultation helps the doctor to understand the expectations of the patient. A filler injection is an outpatient procedure. The area to be treated is numbed with a numbing cream or injections. The filler is injected into the area with syringes with very fine needles. There may be bruising at the treated area. Most of it is usually gone by one or two days. The main benefits of filler injections are the minimal downtime and almost immediate results. Patients can get back to work or other activities soon after treatment.
Gynecomastia or male breast enlargement is a common condition affecting men of all ages. It is a cause of much distress in those affected. Due to the embarrassment, it causes they may avoid situations which reveal the chest deformity. These include places like gyms, swimming pools and places of religious worship.
Corrective surgery for gynecomastia is a short stay procedure. Surgical correction results in definitive and longstanding improvement of this condition. As the enlargement is comprised of both fatty and glandular they are both removed separately. Procedure: During the day of surgery patients have to present at the surgical center with an attendant. This could be a close friend or relative. Once the markings are performed, the surgery is done under general anesthesia. Liposuction is used to remove the fat from the enlarged breast tissue with a small pipe like instruments. The remaining gland is removed directly with the help of a small incision near the nipple. Dressings are placed over sutures and are held in place with the help of paper tapes. A compression garment is placed for reduction of the swelling. Sometimes a drain is placed to help evacuate any fluid which collects at the operated site. First week: Patients are discharged after an overnight stay. They can resume light activities once they reach home. In case a drain has been used it is removed during the first operative visit. This is usually scheduled two days after discharge. During this visit, fresh dressings are applied. After this patients can shower and apply a dressing over the suture line. Suture removal is done at one week. The second week onward: Pressure garment is advised till one month after surgery. Most of the swelling is gone at the end of one week. It is common to have symptoms of abnormal sensation near the scar. This usually resolves in a few weeks without any intervention. Patients can return to light work at the end of the first week. Unrestricted activities like sports can be resumed at the end of one month. Pain after procedure: Gynecomastia correction is usually not associated with significant pain. This is probably due to the liposuction with the administration of local anesthetic mixture. Pain if present is usually well managed with oral medications. Scars: As the incisions placed are very small the resulting scars are small and not readily noticeable. An incision placed within the pigmented part around the nipple (areola) settles very well and is nearly inconspicuous. Most of the operated patients are much relieved to get rid of the excess breast tissue and have an increased level of self-confidence after the procedure. |
AuthorI like to keep it simple. CategoriesArchives
March 2024
Categories |
- Home
-
Cosmetic
- Fat grafting
- Swellings and moles
- Scar revision
- Leukoderma (Melanocyte transfer)
- Hair transplant
- Facial rejuvenation procedures
- Nose job (Rhinoplasty)
- Cleft lip nose correction
- Ear (Otoplasty)
- Lip reduction
- Breast augmentation
- Breast reduction
- Tuberous breasts
- Axillary breasts
- Gynecomastia
- Liposuction
- Brachioplasty (Arm contouring)
- Abdominoplasty (Tummy tuck)
- Female genital rejuvenation
-
Reconstructive
- Contact
- Blog
- Home
-
Cosmetic
- Fat grafting
- Swellings and moles
- Scar revision
- Leukoderma (Melanocyte transfer)
- Hair transplant
- Facial rejuvenation procedures
- Nose job (Rhinoplasty)
- Cleft lip nose correction
- Ear (Otoplasty)
- Lip reduction
- Breast augmentation
- Breast reduction
- Tuberous breasts
- Axillary breasts
- Gynecomastia
- Liposuction
- Brachioplasty (Arm contouring)
- Abdominoplasty (Tummy tuck)
- Female genital rejuvenation
-
Reconstructive
- Contact
- Blog
You can leave us a comment using the contact form below.
We shall get back to you at the earliest.
We shall get back to you at the earliest.
Links
- Face procedures | Rhinoplasty, Otoplasty, Lip reduction, Fat grafting
- Body procedures | Gynecomastia , Breast reduction, Abdominoplasty, Brachioplasty, Liposuction
- Skin procedures | Scar revision, Moles, Leukoderma surgery
Let's be friends !
Follow us at Facebook and Twitter.
Follow us at Facebook and Twitter.
Vectors designed by Freepik
© 2024 Amicus Clinic (Plastic Surgery Centre, Trivandrum). All rights reserved.
© 2024 Amicus Clinic (Plastic Surgery Centre, Trivandrum). All rights reserved.

 RSS Feed
RSS Feed



