|
Scars are an inevitable consequence of injuries. The deeper and more severe the injury, the greater the resultant scar. However, in certain situations, a scar can be unduly prominent. The scar tissue may raise above the surrounding skin. It may also be associated with symptoms such as itching and deformity. Such a presentation is usually suggestive of a hypertrophic scar. What causes hypertrophic scarring? Prolonged healing times can contribute to a hypertrophic scar. In other words, wounds that take a long time to heal are more likely to end up as hypertrophic scars. In some individuals, there is an inherent tendency to have hypertrophic scars. Sometimes milder injuries can end up as very prominent scars in such individuals. Unfortunately, we can't get rid of this tendency of such patients to have prominent scars. What are the treatments available for hypertrophic scars? Certain treatment modalities help prevent and achieve early resolution of hypertrophic scarring. Prevention is recommended in individuals who are prone to such scars. If an individual is prone to such scarring it would be wise to deliberate before going for procedures such as tattoos or piercings. It is also better to bring this to the attention of a surgeon before elective surgery. The modalities used for prevention and treatment are similar. These include the application of silicone sheet, pressure garments and intralesional injection of immunomodulatory substances. These are usually carried out for prolonged periods for sustained benefits. Surgery has a limited role in the treatment of hypertrophic scars. Can hypertrophic scars be prevented? Some measures can reduce the likelihood of such an outcome. They include steps to hasten wound healing. Wounds that take more than two weeks to heal have a higher likelihood of ending up as hypertrophic scars. In individuals who have a history of prominent scars use of silicone sheets and pressure, garments are recommended. In certain situations, we also recommend the use of intralesional agents. What is the role of surgery in the treatment of hypertrophic scars? After treatment, the hypertrophic scars usually flatten out and become atrophic. Atrophic scars appear as thinned out and shiny. Surgery is a good option for the management of atrophic scars. The surgical procedures for atrophic scars include scar revision and fat grafting. To learn more about scars and various treatments please click here. In this age, it is almost essential to look lean and fit. Lean is associated with health and vitality. It is common knowledge that a large waistline is contributed by excess fat deposits. And because of this many individuals turn to plastic surgery for liposuction as a solution to this problem. However, all cases of the protuberant belly cannot be tackled by plastic surgery.
Excess deposits of fat can be found in many places within the abdomen. They are found in the layer between the skin and the muscles of the abdominal wall. This is the layer that can be pinched between the fingers as a roll. Fat is also deposited deep inside the muscle layer. This fat is referred to as visceral fat and is found in association with our gut and the area behind it. Other than fat deposits, laxity of the abdominal wall can contribute to protuberance. Laxity of the abdomen can be seen as a result of changes due to aging and pregnancy. A separation of the abdominal muscles in the midline, known as divarication is often seen in such individuals. Some of the above-mentioned deformities can be tackled with the help of plastic surgery. The modalities used for correction include procedures such as liposuction and abdominoplasty. Liposuction involves suction of fat with the help of small cannulas inserted through the skin. Fat is aspirated with the help of a vacuum producing device. Advantages of this procedure include the treatment of relatively large areas with the help of tiny incisions. Patients usually recover fast and are ambulant as soon as they are awake from the effects of anesthesia. It does not involve a prolonged stay in hospital. Liposuction targets only fat that is superficial to the abdominal muscles. We are not able to access the deep or visceral fat with liposuction. Another limitation of liposuction is that it does not address the laxity of the abdominal wall or skin. Abdominoplasty translates into reshaping the abdomen. During an abdominoplasty, we tighten the layer of the muscles. This helps tackle the laxity of the muscle layer. Liposuction is often carried out as a part of abdominoplasty. Liposuction is used to reduce the fat deposits on the flanks and in the upper abdomen. This improves the appearance and increases the safety of the procedure by limiting the areas of surgical dissection. We also reduce the excess skin as an ellipse from the lower abdomen. The rest of the skin is draped to result in a tighter-looking abdomen. As with liposuction, abdominoplasty can't address the visceral fat. A clinical examination helps reveal the cause of the deformity and arrive at a treatment plan. Ideal candidates for both the procedures include patients close to their ideal body weight. They should be non-smokers and have reasonable expectations about the procedure. It is also important to be aware of what can be achieved using plastic surgery. We can achieve a reduction in the fat deposits that are external to the muscles and obtain a tightening of the muscle-fascia layer and skin. Plastic surgery does not address the visceral fat. And because of this, patients need to adopt a dietary and exercise regimen to maintain appropriate levels of visceral fat. Macromastia or disproportionately enlarged breasts in females is not an uncommon condition. Treatment is often sought for physical and mental effects of this condition. Symptoms due to the heavy breasts include shoulder and neck pain, grooving of the skin due to garments and, maceration of the skin under the breast folds. Patients are often embarrassed due to this condition and find difficulty in getting suitable clothes.
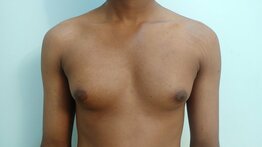
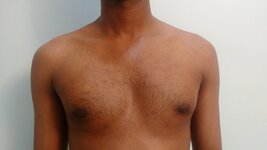
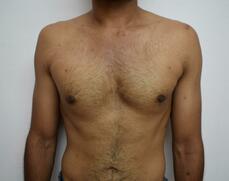
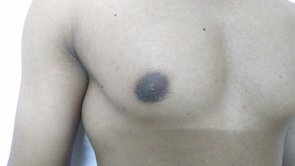
Reduction mammaplasty (breast reduction surgery) is a very effective procedure to address macromastia. It helps patients to achieve a reduction in the size of the breasts as well as an improvement in the appearance of the breasts. It also allows us to tackle mild breast asymmetries and help position the nipple and areola to a more aesthetic position. When the procedure is carried out in a patient previously operated for macromastia, it is known as secondary reduction mammaplasty. The following may be some of the reasons to carry out a secondary breast reduction surgery. Patients sometimes report that the breasts have increased in size after the first surgery and desire a further reduction in the size of breasts. They may be bothered about the scars associated with the previous surgery. In certain situations, patients may want to improve the position of the nipple in relation to the rest of the breast. The decision to explore a secondary breast reduction procedure is taken after careful discussions with the patient. Some of the important points factored into the decision making include, the time elapsed after the first surgery, the type of reduction carried out previously, scarring tendency of the individual, etc. The procedure is usually carried out as a short stay procedure in a hospital setting under general anesthesia. Post-procedure patients have to comply with the use of pressure garment and care of the breasts. In cases of secondary correction, patients are usually very familiar with the process of recovery. Breasts are an important part of the body image of a woman. Disproportionately large breasts result in significant morbidity among some of the affected individuals. Reduction mammaplasty is a powerful technique to help those affected by this condition. Click here for more details about reduction mammaplasty. Hello, is this the plastic surgery clinic? Yes. Do you perform rhinoplasty? Yes, we do. What is the cost of rhinoplasty? We need to see you before we comment on the treatment plan or the cost. Is it possible to give a rough estimate? ……. We tend to have the above conversation multiple times. Sometimes rhinoplasty gets replaced by another procedure such as liposuction, fat grafting or something else. I thought of elaborating more about our resistance to comment on treatment costs before seeing the patient. Imagine a person with a desire to build a home. Not an apartment in a high-rise, but someplace on a piece of land with a small garden. Such a person would have certain ideas about size, location, immediate vicinity, style, etc. And if there is a lack of clarity related to these aspects she would assume that she would be guided by an expert. Now let's imagine another conversation. Hello, is this the builder's office? Yes. Do you build homes? Yes, we do. What is the cost of building a home? …….. We find both these conversations very similar. Because we are dealing with situations in which making plans would not make sense without a good grasp of what the customer needs. In other words, both cosmetic surgery and building a home are highly customized endeavors. There are a lot of variables which need to be sorted out or understood before we finalize a plan. In both cases, the expert brings to the table his or her expertise. Once a plan is finalized it is reasonable to arrive at the cost. It is nearly impossible to follow a cookie cutter approach in cosmetic surgery. Let me give an example. Let us assume an individual seeking rhinoplasty. Following a clinical examination and discussion, we usually arrive at a treatment plan. A plan found suitable for one person may be quite different from a plan for another individual. One may require a short procedure lasting one hour whereas the other may require something much more complex lasting six hours. The cost, in turn, depends on the complexity and duration of a treatment procedure. Like an architect who seeks input from her client, we give a lot of importance to input from our patients. This more so in cosmetic surgery when compared to other surgical specialties. Because of this, a similar looking deformity may get treated using different techniques. One individual may be satisfied with a simple correction whereas another may be keen on a more exacting remedy. This again reflects on the cost of the procedure. This sort of variability in treatment options applies to almost procedures in cosmetic surgery. Because of these reasons we hesitate to comment on any treatment plan when certain pictures or images are sent to us. We do get an approximate idea of the deformity with the images, but in the absence of a discussion with the patient, it does not make much sense to decide on a treatment plan. Also, a clinical examination gives a lot of important and useful information relating to the management of the condition. These are not otherwise apparent by inspecting images of the body part. To give an example, in rhinoplasty we get to assess aspects like the thickness of the skin and soft tissue, structural support, status of the nasal cavity as well as nasal obstruction with a clinical examination. These can't be inferred from the pictures. It may sometimes be possible to give an estimate of the cost when a procedure is simple or straightforward. This applies to procedures like excision of a mole with a straight-line closure or repair of an earlobe cleft. This can also apply to procedures like hair transplant when the cost can be correlated in terms of a smaller unit say, cost per follicular unit. All of the above reasons lead to a reluctance to comment on the cost of a procedure without a clinical examination and discussion. I suppose similar reasons would also apply to those who seek to get a home built somewhere. Gynecomastia is an enlargement of the male breast tissue. This enlargement can be of one or both sides. In cases of bilateral involvement, one side can be affected more than the other, leading to an asymmetrical appearance. Mild cases of asymmetry are common. But in certain cases, the difference between the two sides can be readily noticeable. The asymmetry can be as a result of two causes, namely, a difference in the amount of breast tissue or changes as a result of the underlying chest wall and muscles. The treatment strategies for managing the asymmetry depends on the underlying cause. Usually, the reason is apparent during a clinical examination. In the case of asymmetry arising due to the difference in the size of the breast tissue, the treatment involves liposuction and direct glandular excision. We take care to leave behind equal amounts of subcutaneous tissue at the end of the procedure. A more enlarged gland will require a longer time for adequate skin recoil. Such a gland may also have a longer duration of postoperative firmness. In most cases, adequate symmetry is achieved with the passage of time. In cases of asymmetry due to underlying chest muscles, unfortunately, nothing much can be done to correct the difference at the time of surgery. We bring this to the notice of the patient during the consultation. Usually, such differences in chest muscles arise from altered posture and position during strength training exercises. It is recommended that individuals seek help and guidance from an expert physical trainer for the correction of the posture and technique. Gynecomastia surgery is essentially a cosmetic procedure and the goal of undertaking a correction is to minimize the effect of the deformity. Wide variations occur in the presentation of this condition. Asymmetry is a commonly seen variant, even though severe asymmetry is uncommon. In cases of asymmetry, it is important that individuals understand the reason and the role of different treatment strategies to tackle the same. For more information about gynecomastia and related topics, click here. An individual with asymmetry due to difference in the size of the gland. The right side is bigger compared to the left. Asymmetry due to the difference in the size of the underlying muscles. The left pectoralis major is more developed when compared to the right.
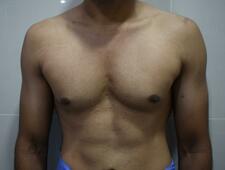
As in all surgical procedures, the operated areas following gynecomastia correction take time to settle down and return to the preoperative suppleness. Gynecomastia correction is a commonly done procedure in our practice. Correction is indicated if the individual is affected by the appearance of the chest. Patients report a sense of embarrassment and shame due to the feminine appearance of the male chest. The goal of the surgery is to enhance the appearance of the chest.
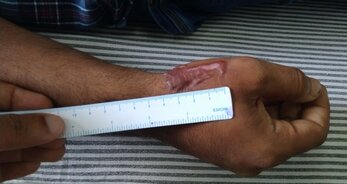
Most cases of gynecomastia are done under general anesthesia using a combination of liposuction and direct glandular excision. Most patients are sent home after an overnight stay and make an uneventful recovery. There are no restrictions on sports or any other heavy exertion after a month. Even though there is a significant improvement in appearance during the initial weeks following surgery, patients should also be familiar with certain late changes that occur with healing. These are often a part of the normal process of healing. Being aware of these changes helps reduce anxiety among some patients. The scar used for gland removal is a curve within the areola. The areola is the pigmented skin around the nipple. Scars within the areola tend to settle well when compared to scars at the junction of skin and areola or those in the surrounding skin. As with all scars in the postoperative period, the scars tend to contract. This effect is marked between 6 to 12 weeks. Following this, they again elongate and become softer. This transient contraction can result in a feeling of induration and pushing up of the skin around the nipple. We refer to this phenomenon as a trapdoor deformity. In most cases, nothing has to be done as the condition settles once the scar elongates and becomes softer over the next few months. Even though the external scars are limited the operated areas involve the front and the sides of the lower chest. These areas can also undergo changes similar to the overlying scar. Some of the patients report the onset of a firmness appearing around one month following the procedure. This leads to anxiety as some individuals interpret this as recurrence of gynecomastia. As with the overlying scar, this is usually as a result of transient contraction of the wound bed. Over the next few months, the swelling and firmness subside. The tissues may take up to eight months to become supple. We reassure our patients to wait that long before they can appreciate the final results. The formation of a scar is an essential part of healing. Even though a temporal sequence is predictable, in some cases these changes are more pronounced. Being aware of these changes and waiting it out is often the only remedy. To learn more about gynecomastia, click here. Gynecomastia correction is a commonly done cosmetic procedure. Surgery is indicated in case the affected individuals are bothered about the deformity. An effective correction is associated with improvement in self-confidence.
Most cases are done under general anesthesia in a hospital setting. We reserve local anesthesia for the mild variants with only gland enlargement. Gynecomastia is usually associated with an increase in fatty and glandular tissues. The incisions and the resulting scars depend on the tissues being tackled during gynecomastia correction. Less commonly, there can be a significant excess of skin. 1. Fat is removed with the help of liposuction. During liposuction small tubes are used to suck out fat. An advantage of liposuction includes the ability to treat large areas with the help of very small wounds. These incisions are usually not sutured and heal very rapidly. Liposuction also contributes to postoperative comfort during recovery. This is due to the infiltration of the anesthetic solution during the procedure. 2. The gland is removed with the help of an incision placed inside the areola. The areola is pigmented skin immediately surrounding the nipple. The wound is closed with sutures. These sutures are removed around 7 days following surgery. The areolar scar usually settle very well. The exceptions would be seen in certain patients prone to prominent scars. 3. Skin is usually not removed during correction of gynecomastia. Skin excess can be seen in long-standing severe gynecomastia and those with massive weight loss. These individuals present with droopy or hanging breasts. Removal of the underlying gland and fatty tissues helps the skin to recoil. This can take as long as one year. For this reason, we usually wait for a year before planning any skin tightening or removal procedure. Depending on the severity of excess skin, incisions may be confined to the junction between the areola and skin or may extend downwards and laterally towards the sides of the chest. In most cases presenting for gynecomastia, we do a combination of liposuction and gland removal with an areolar incision. These scars are associated with high patient satisfaction rates. Skin removal surgery is very uncommonly done in our practice. learn more about gynecomastia here. Macromastia is a condition with disproportionately enlarged breasts in women. This can be a cause for significant emotional and physical distress in those affected by this condition. Reduction mammaplasty is a surgical condition to reduce the size of the breasts by making it more proportionate to the rest of the body.
The cause of macromastia is usually undetermined. It can be as a result of a change in levels of hormones and sensitivity of the tissues to hormones. There can be an enlargement of the gland, fat and excess skin in this condition. Medicines do not have a significant role in the treatment of macromastia. Surgery is the mainstay of treatment of this condition. Macromastia can result in physical symptoms such as neck and backache, skin grooving and skin rashes over the folds below the breasts. Patients may find it difficult to perform strenuous exercise and other physical activity. Individuals with this condition also find it difficult to get appropriately sized clothing. Macromastia can result in emotional distress and a feeling of embarrassment and social inhibition. Surgical correction is achieved by reduction mammaplasty. This is aimed at reduction of the size the breasts, and reshaping it to give a more pleasing appearance. The areola (pigmented skin around the nipple) is also reduced in diameter in case they are enlarged. The scars associated with this procedure are confined to the skin at the junction between the areola and breast and a vertical limb towards the undersurface of the breast. In most individuals, the scars settle well. Reduction mammaplasty is carried out in the hospital setting under general anesthesia. Patients are admitted overnight after the procedure and discharged home the next day. Discomfort is controlled with the help of pain medications. Patients are not confined to bed and are able to carry out daily activities like showering from the next day. Most patients resume work in a week. Strenuous activities can be started after a month. Benefits of reduction mammaplasty are physical, emotional and social. After reduction mammaplasty, individuals report the absence of back and skin symptoms. Patients find it easier to perform strenuous activities. Patients have increased levels of self-confidence and are no longer embarrassed by this condition. For more information, visit us at: https://www.amicusclinic.in/breast-reduction No. It can't be.
Working out at the gym has health benefits. One of it would be to get a muscular and aesthetic chest. And for the same reason, it is hoped that lifting weights would help get rid of the excess breast tissue. The reason why it does not help has to do with the tissues which are responsible for gynecomastia. Gynecomastia is comprised of glandular tissue, surrounded by varying amounts of fat. The muscle which gives definition to the chest is pectoralis major and is found behind the breast tissue. Working out at the gym and lifting weights can augment the size of the muscles. This can lead to a more anterior (forward) position of the overlying breast tissue. So paradoxically, lifting weights can make the deformity more obvious. Losing weight can have beneficial effects on the appearance of gynecomastia. This acts by reduction of the fatty tissue. This will lead to an overall reduction in the size of the breast tissue. However, losing weight does not reduce the glandular tissue found beneath the nipple-areola. So there would be a persistence of the puffiness of the nipple region. So what gets rid of gynecomastia? In most cases, the answer would be surgery. Due to technical refinements, it is possible to treat this condition with very small incisions. Fat around the gland is treated with liposuction and the gland is removed with a small incision in the areola (the dark skin surrounding the nipple). In most individuals, these lead to very fine scars. The goal of gynecomastia correction is improved aesthetics of the chest. There is a role for medical intervention in cases of gynecomastia which are secondary to abnormal levels of certain hormones. To conclude, cosmetic surgery offers a definitive cure for this condition which can't be attained by pumping weights at the gym. Otherwise, bodybuilders would have been immune to this condition. For more information about gynecomastia, click here. Scars are common. We start our lives with an umbilical stump that matures into a scar. But since everyone has one we do not seem to mind having it.
Scar looks and feels different because it is composed of tissues which are different. Due to this scar has different biomechanical and light reflecting properties. And at times it can lead to significant distress in those with these scars. A scar is a living tissue that changes its composition over a period of time. We know this as scar remodeling. Many therapies exist to favorably alter the appearance of the scar. They vary in their simplicity and invasiveness. There are certain activities that can be done by anyone to make scars better. We commonly ask our patients to perform these to have a better-looking scar. These would be,
In most instances, scar remodeling favorably affects the scar. Scar remodeling is greatest during the initial one to two years. This usually leads to more supple and flattened scars. Because of this, we tend to postpone any surgical scar treatments until one to two years since we would like to reap the benefits of scar remodeling. To conclude, though one can't completely eliminate scars, it is possible to influence the outcome of scars by means of simple techniques that be done by the patient. With compliance, a patient can end up with more acceptable scars. |
AuthorI like to keep it simple. CategoriesArchives
March 2024
Categories |
- Home
-
Cosmetic
- Fat grafting
- Swellings and moles
- Scar revision
- Leukoderma (Melanocyte transfer)
- Hair transplant
- Facial rejuvenation procedures
- Nose job (Rhinoplasty)
- Cleft lip nose correction
- Ear (Otoplasty)
- Lip reduction
- Breast augmentation
- Breast reduction
- Tuberous breasts
- Axillary breasts
- Gynecomastia
- Liposuction
- Brachioplasty (Arm contouring)
- Abdominoplasty (Tummy tuck)
- Female genital rejuvenation
-
Reconstructive
- Contact
- Blog
- Home
-
Cosmetic
- Fat grafting
- Swellings and moles
- Scar revision
- Leukoderma (Melanocyte transfer)
- Hair transplant
- Facial rejuvenation procedures
- Nose job (Rhinoplasty)
- Cleft lip nose correction
- Ear (Otoplasty)
- Lip reduction
- Breast augmentation
- Breast reduction
- Tuberous breasts
- Axillary breasts
- Gynecomastia
- Liposuction
- Brachioplasty (Arm contouring)
- Abdominoplasty (Tummy tuck)
- Female genital rejuvenation
-
Reconstructive
- Contact
- Blog
You can leave us a comment using the contact form below.
We shall get back to you at the earliest.
We shall get back to you at the earliest.
Links
- Face procedures | Rhinoplasty, Otoplasty, Lip reduction, Fat grafting
- Body procedures | Gynecomastia , Breast reduction, Abdominoplasty, Brachioplasty, Liposuction
- Skin procedures | Scar revision, Moles, Leukoderma surgery
Let's be friends !
Follow us at Facebook and Twitter.
Follow us at Facebook and Twitter.
Vectors designed by Freepik
© 2024 Amicus Clinic (Plastic Surgery Centre, Trivandrum). All rights reserved.
© 2024 Amicus Clinic (Plastic Surgery Centre, Trivandrum). All rights reserved.

 RSS Feed
RSS Feed



