|
Emulsified fat grafting is an innovative technique that may help individuals experiencing hair loss. This minimally invasive procedure involves taking fat from the patient's own body, processing it, and then carefully injecting it into the scalp.
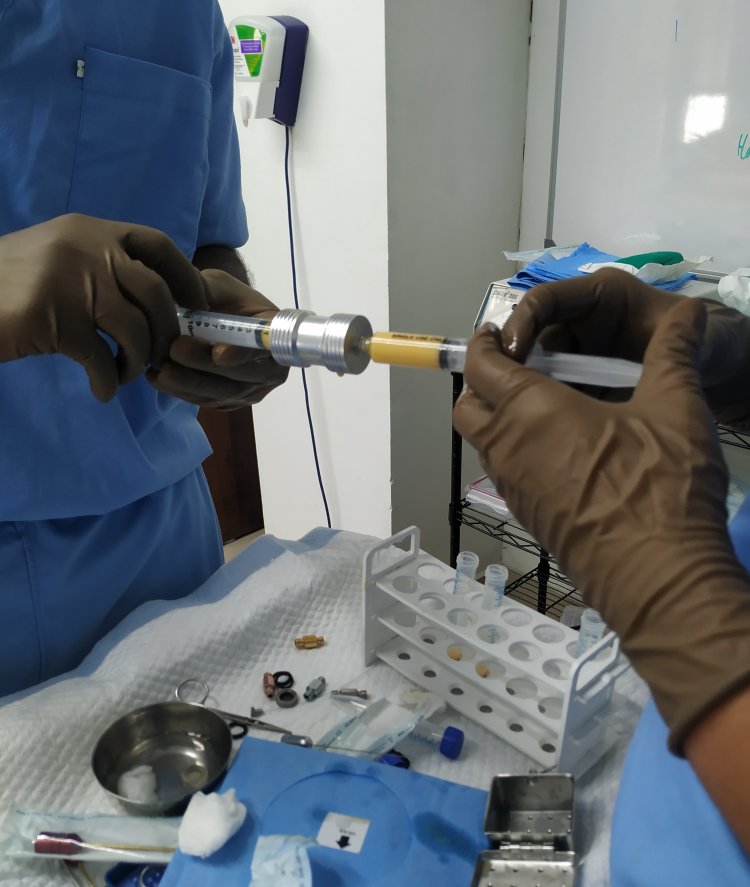
The process starts by gently extracting fat from an area like the abdomen or thighs using a small, thin cannula. The harvested fat is then prepared for reinjection. The prepared fat is then injected into the scalp using fine needles, targeting the areas affected by hair loss. One key advantage of emulsified fat grafting is the potential for longer-lasting results compared to other treatments like platelet-rich plasma (PRP) injections. The injected fat can help stimulate new hair follicle growth and improve blood flow to the scalp, potentially leading to better hair density and thickness. Emulsified fat grafting is typically an outpatient procedure, meaning the patient can go home the same day. Recovery time is generally minimal, with little to no downtime reported by patients. The video in Malayalam gives an overview of the topic.
0 Comments
Structural fat grafting is a procedure that involves the transfer of fat cells from one part of the body to another. It is done because of various benefits such as improved volume of the treated areas, and tissue regeneration. Emulsified fat grafting is a different procedure during which the tissue is transferred without viable (living) adipocytes (fat cells). The emulsification helps get rid of any viable (living) fat cells.
Why is emulsified fat grafting done? Unlike structural fat grafting, emulsified fat grafting does not result in increase in the volume of the treated areas. Instead, it leads to an improvement of the regenerative properties of the tissues. This results in improvement in the texture of skin, scars, or enhanced healing of wounds. How does emulsified fat grafting work? The fat containing tissues in have fat cells and supporting cells that help in growth and regeneration. The supporting cells are referred to as ADSC. During harvest, both adipocytes (fat cells) and the supporting cells are obtained together. The adipocytes or the fat cells are removed by mechanical disruption. The supporting cells are not affected by this process. These are injected into the body for their beneficial properties. Due to the absence of adipocytes, emulsified fat grafting does not lead to an increase in the volume of the grafted part. What are the various applications of emulsified fat grafting? Emulsified fat grafting helps the tissues in growth and repair. The various applications include
How is emulsified fat grafting performed? Emulsified fat grafting is usually carried out under local anesthesia as an outpatient procedure. The common areas for the harvest of fat are the abdomen or thighs. Small volumes are needed for this procedure. The harvested fat is then processed. The emulsified fat is then injected with the help of fine needles into the treated area. The treated areas are left open. The donor areas are treated with simple dressings that are removed after two days. What is the recovery from emulsified fat grafting? The donor area will have some firmness and induration that subsides over the next few weeks. The treated areas can show some swelling that subsides over days to weeks. The improvement in the texture of the skin takes a few weeks to become noticeable. In case of fat grafting into wounds, the following weeks may show accelerated healing. The changes in hair growth in case of injections for male pattern baldness may take a few weeks to become visible. What are the advantages of emulsified fat grafting? Emulsified fat grafting is beneficial across a variety of indications. It is also attractive since it is done as an outpatient procedure with a rapid recovery. The beneficial effects of the procedure are also long lasting. Recently I was asked about home remedies for scars. I usually don't suggest any. Some of my patients describe the benefits of certain types of oils. I do not promote or recommend the use of any particular type of medication on settled scars. Also, I do not caution them against the use of any particular oil.
But there is a definitive role of certain conservative measures that can help improve scars. They are not advised in all cases. The effect of these measures should be understood by those using these. They should be carried out as per the guidance of the treating doctor. Some of the commonly advised measures for scars include the following,
Certain other non-surgical measures are carried out to help improve a scar. Examples would include laser and intralesional injections. But these are carried out by a doctor. Even though home remedies may not have many roles for optimizing scars, certain conservative measures are frequently advised. Most of them help in scar remodeling. Removal of small skin swellings is common in our practice. Patients usually get them removed for the following two reasons,
In most cases, removal of the swelling is a simple and straightforward procedure. It is usually carried out under local anesthesia in adults. Patients usually go home after the procedure and follow up as an outpatient for inspection of the wound and suture removal. In case a biopsy was done, the case is reviewed once again after the biopsy report. One of the reasons why patients come to a plastic surgeon is due to the concerns relating to the postoperative scars. In other situations, the referrals are due to the relative difficulty in obtaining closure in regions such as folds near the eyes, mouth, or nose. In the majority of cases, we remove the swelling with a small margin of skin. This can vary based on the type of swelling. Some of them mandate a narrow margin while others require a wider margin. This is based on clinical presentation. Additional pre-operative investigations may be ordered in some cases. The removal of swellings consists of two parts. First is the removal, resulting in a wound. And the second is the closure wherein the tissues are approximated to achieve optimal healing. In most cases, the second part is done with a straight line closure. However, this may not be possible in certain situations. This may be due to wide separation between the wound edges, or proximity to regions such as eyes, nose, or mouth. In such situations, we resort to techniques such as skin grafts or flaps. We make intelligent use of neighboring or distant tissues to effect good closure. Some of the swellings may not arise from the skin. They may originate from other structures like fat. Removal of such swellings gives us some liberty concerning the placement of the surgical wounds. Some orientation of the surgical scars may be associated with a better outcome compared to others. Knowledge about the orientation of optimal incision lines helps us give a better looking postoperative scar. Removal of these swellings is associated with a good outcome in most individuals. A small subset of individuals tends to have problem scars. It is usually possible to predict the scarring tendency of an individual by observing previous scars on the body. Two possible adverse outcomes related to the tendency for stretched out scars and hypertrophic scars. Though scar hypertrophy can be treated, patients need to be aware of such a possibility. Removal of skin swellings is a minor and safe surgical procedure with very little downtime. With good technique, it is possible to get good outcomes in most individuals. For more information on skin procedures, click here. Hair transplant is a surgical procedure for redistribution of hair from areas of relative abundance to those with deficiency. It is most often carried out for male pattern baldness (MPB). In MPB, the hair of the posterior (back) of the scalp is relatively spared when compared to the hair in front of the scalp. The word, 'relatively' is important since the hair in the posterior part of the scalp is not completely unaffected by the changes in MPB. However, this property of relative sparing of the posterior scalp hair in MPB continues even after grafting (transplant).
Hair shafts occur as small groups called follicular units. During a hair transplant, a follicular unit is removed from the donor area (usually the posterior scalp) and implanted at the recipient area (usually the front of the scalp). A follicular unit may contain one, two or three hair shafts. The number of follicular units transplanted in a procedure depends upon the donor and recipient areas. Male pattern baldness usually requires the transfer of a large number of grafts. This is in contrast to the small numbers required for hair loss associated with small scars. As mentioned previously, the posterior (back) part of the scalp is usually used as a donor area for hair transplants. Less preferred donor areas include beard and body hair. In certain individuals, the posterior scalp hair may be inadequate as a source for donor grafts. This can be due to the progress of MPB. This is observed as reduced density (hair follicles per square cm) and thinning (miniaturization) of hair follicles. It can also be as a result of a previous harvest of hair follicles during a hair transplant. An individual with a poor donor area also tends to have an advanced stage of MPB. In spite of these challenges, it is possible to improve upon the appearance of those with a poor donor area. In such a situation we try to achieve improvement with the help of fewer grafts. Frontal forelock occupies the portion behind the central part of the forehead. Many individuals with advanced male pattern baldness tend to retain hair in this region. A relatively full forelock does not give an unnatural look in an individual with advanced hair loss. The forelock helps frame the face when an individual is observed from the front. It would be the part of the scalp that would be visible as a person steps out of an elevator. Increasing the density in the forelock region would require lesser grafts when compared to the rest of the scalp. In patients without donor deficiency, other areas that are addressed include the hairline and mid-scalp. These occupy the area adjoining the forelock. The crown is given lesser importance when compared to the previously mentioned areas because of the lesser aesthetic significance and the requirement of a large number of grafts. Salvaging the remaining hair follicles is also important in a person with MPB. MPB is usually a progressive condition and left untreated many can progress to more advanced stages of baldness. This is especially true in the case of younger individuals in whom the hair loss has not stabilized. Preservation of remaining hair follicles is achieved by means of medications. These medications include nutritional therapy, topical Minoxidil, and Finasteride. It is important for individuals to make an informed decision about the use of these medications. They should be taken for long periods for adequate results. Male pattern baldness with poor donor areas offers some challenges for hair restoration. But often it is possible to improve upon the appearance with the help of medications and a limited hair transplant. For more information on hair transplant please visit, https://www.amicusclinic.in/hair-transplant Male pattern baldness (MPB) is a progressive condition. The extent of baldness in MPB is described using Norwood classification wherein I is the mildest and VII is the most severe. Male pattern baldness (MPB) begins with the recession of the hairline in front and progresses to involve the hair on the top of the head (mid-scalp) and the back of the head. It is difficult to predict the extent (severity) to which a person with MPB will lose hair and the speed or rate at which the hair would be lost.
We adopt two strategies for the management of MPB. They include those for the prevention of hair loss and those for redistribution of the hair follicles. The former involves medications and the latter is achieved with hair transplantation (surgery). With the progress of MPB, there are certain changes observed in the appearance of the hair shafts. They become smaller in length and diameter. Hair shafts in the scalp occur in bunches of single, two, three or four shafts. These are referred to as follicular units (FU). In MPB, the average number of shafts in an FU reduce with a predominance of singles and doubles. The number of hair follicular units in a given area (hair shafts per square cm) reduces with the progression of baldness. All of the above changes contribute to the seemingly less dense look with increased visibility of the scalp. With preventive strategies, we are trying to halt these changes found in the scalp. Prevention is important because this alone tries to preserve the total number of follicular units. Hair transplantation (HT) on the other hand is essentially a redistribution of FU. Hair transplantation does not do anything for preventing the progress of MPB. Both these modalities are adopted together in the management of MPB. The relative importance of prevention versus surgery in a given individual depends on the clinical presentation. In cases of early MPB with ongoing loss, prevention is more important when compared to individuals presenting with a stable pattern of MPB (without significant ongoing loss). In other words, the treatment plan is customized based on the findings seen in an individual. Prevention is undertaken using medications. These include oral and topical (local application) medicines. Oral medications include, nutritional therapy wherein nutritional supplements are given regularly to take care of the nutritional deficiencies associated with hair loss. The supplements include vitamins, minerals, amino acids, and essential fatty acids. Another oral medication for MPB is Finasteride. Finasteride blocks the conversion of testosterone to dihydrotestosterone (DHT). In MPB, the hair follicles in the loss prone area of the scalp have an abnormal sensitivity to DHT. The effect of DHT mediates the changes observed in MPB. Finasteride thus helps reduce the effect of DHT on the hair follicular cells. Finasteride is uncommonly associated with loss of libido and associated symptoms. Studies have reported an incidence of these effects of one in fifty individuals. Despite this Finasteride is an important medication for the management of MPB. Topical Minoxidil is another useful drug in MPB. Minoxidil was first introduced as an oral medicine for the treatment of hypertension. It was soon found to have positive effects on the growth of hair. Minoxidil comes in various strengths. Minoxidil is usually applied twice daily on the scalp. Minoxidil should be allowed to have a scalp contact time of more than an hour before it is washed away. Individuals are asked to apply minoxidil after drying hair following a shower. Minoxidil is useful in the mid-scalp region. Continuous use over a few months is needed before optimal results are seen. Preventive strategies are important in the management of MPB. They help preserve the existing hair follicles. The use of the medications also needs a high level of motivation and they give the best results with continued use. Both preventive medicines and surgery play an important role in achieving a good outcome in MPB. Both of these strategies are complementary. One can't substitute the other. In other words, a good transplant can't reduce the importance of steps for the prevention of hair loss. Scars are an inevitable consequence of injuries. The deeper and more severe the injury, the greater the resultant scar. However, in certain situations, a scar can be unduly prominent. The scar tissue may raise above the surrounding skin. It may also be associated with symptoms such as itching and deformity. Such a presentation is usually suggestive of a hypertrophic scar. What causes hypertrophic scarring? Prolonged healing times can contribute to a hypertrophic scar. In other words, wounds that take a long time to heal are more likely to end up as hypertrophic scars. In some individuals, there is an inherent tendency to have hypertrophic scars. Sometimes milder injuries can end up as very prominent scars in such individuals. Unfortunately, we can't get rid of this tendency of such patients to have prominent scars. What are the treatments available for hypertrophic scars? Certain treatment modalities help prevent and achieve early resolution of hypertrophic scarring. Prevention is recommended in individuals who are prone to such scars. If an individual is prone to such scarring it would be wise to deliberate before going for procedures such as tattoos or piercings. It is also better to bring this to the attention of a surgeon before elective surgery. The modalities used for prevention and treatment are similar. These include the application of silicone sheet, pressure garments and intralesional injection of immunomodulatory substances. These are usually carried out for prolonged periods for sustained benefits. Surgery has a limited role in the treatment of hypertrophic scars. Can hypertrophic scars be prevented? Some measures can reduce the likelihood of such an outcome. They include steps to hasten wound healing. Wounds that take more than two weeks to heal have a higher likelihood of ending up as hypertrophic scars. In individuals who have a history of prominent scars use of silicone sheets and pressure, garments are recommended. In certain situations, we also recommend the use of intralesional agents. What is the role of surgery in the treatment of hypertrophic scars? After treatment, the hypertrophic scars usually flatten out and become atrophic. Atrophic scars appear as thinned out and shiny. Surgery is a good option for the management of atrophic scars. The surgical procedures for atrophic scars include scar revision and fat grafting. To learn more about scars and various treatments please click here.
Surgical scar revision is a commonly requested procedure. The changes that can be achieved include:
1. Wide scars can be narrowed. 2. Long scars can be broken down into non-linear zig-zag pattern. This reduces the deformity. They become less readily observable. 3. Scars can be made to lie along natural lines and creases. Thus making them less obvious to an onlooker. 4. Contracture release. Contractures are deforming scars across mobile parts of the body. Contracture release leads to restoration of function of the affected body part. 5. Improvement of texture, color and contour mismatch. These procedures are associated with improvement of body image and self esteem. Learn more about scars here As in all injuries, burns end up as scars. The deeper burns usually give rise to problem scars. These scars can be a cause of disability and impair quality of life of the affected individual. It can lead to problems relating to self-esteem. However, it is possible to improve these scars with the help of restorative surgery. This forms one of the most rewarding specialties of plastic surgery. Restoration means an improvement of both the form and function of the affected part. How do burn scars lead to impairment of function? Scars differ from the native tissue it replaces. They are less elastic and tend to contract with time. Due to this intrinsic property of contraction, scars reduce the movement of structures associated with it. For example, scars stretching across the front (anterior surface) of the elbow can reduce the ability to straighten out the elbow. This leads to a reduction in function of the affected upper limb. In a manual laborer, this can mean the loss of ability to earn his/her livelihood. Scars also look and feel different compared to the unaffected (native) skin. This causes disfigurement. Deformity due to scars can make an individual shun social encounters. What are the indications for surgery for burn scars? They mainly done for two reasons: 1. Functional: When the scar impairs the function of the affected part. Burns affecting the hand may prevent the individual from using the part. With surgical treatment, it is possible to regain useful function of the hand. 2. Cosmetic: Scars can result in deformities. It is usually possible to surgically modify them and improve their appearance. Who are good candidates for burn scar surgery? Good candidates include those who are in good health and have reasonable expectations about the corrective surgery. When does one undergo surgical correction of burn scars? Scars are living tissues which undergo change in a appearance and texture with time. This is sometimes referred to as maturation of a scar. This can around eighteen months and surgery for scars are undertaken once the scars mature. However, in certain instances when the scars are associated with severe functional problems they are corrected earlier. For example, the involvement of the eyelids with scars can result in an absence of eyelid closure. This can lead to ulceration of cornea and blindness. In such a situation scars are treated without waiting for the scars to mature. What are the techniques used in scar surgery? Generally, the scars are cut and the resulting defect (gap) is covered either with neighboring tissues (local flaps) or skin grafts. The exact technique chosen depends on the deformity, treatment options and aesthetic and reconstructive goals of the patient. It is often possible to treat a deformity by more than one technique. Some of the procedures include: Skin grafts: These involve the transfer of the outer layers of the skin to cover a wound elsewhere. The area from where the grafts are obtained heal by itself. Grafts are an attractive option since they are abundantly available. Skin grafts tend to undergo contraction in the postoperative period. Because of this use of splints and pressure garments are important during the postoperative period. Flaps: They are tissues with the associated blood vessels transferred for coverage of a defect. They provide thicker tissues compared to skin grafts. Flaps closely mimic the native tissue in appearance and texture. Thus, they are usually aesthetically superior when compared to skin grafts. Flaps do not contract like skin grafts and once the wounds heal they are easier to manage and do not require rigorous use of splints. Tissue expanders: These are devices which are placed surgically underneath the skin adjacent to a scarred area. During the follow-up visits, they are progressively filled with saline. The inflation of the expanders causes the overlying tissues including skin to get stretched. Once a critical volume is achieved the expanders are removed and the extra skin is used to cover the scarred area. The advantage of such a procedure is that they provide tissues which bear a close resemblance to the native (original) tissue. They are frequently used to treat scars of the scalp. The use of adjacent scalp tissue enables the scar the be replaced with hair-bearing skin. Serial excision: Due to the size of a scar it may not be possible to close the wound edges after removal of the scar. During serial excision, this process is done in stages when a part of the scar is removed during each step. This takes advantage of the increased laxity of the tissues as they respond to the increased tension at the operated site. The advantage of serial excision is that they help narrow a broad scar without the use of additional grafts or flaps. What type of anesthesia is used for burn surgery? Surgery for burn scars is done under local or general anesthesia. General anesthesia is used in children and in adults when the area being treated is extensive. Local anesthesia is used in adults when the area affected is small. What is the recovery following a burn scar surgery? Burn scar surgery is usually performed as a short stay procedure. Patients can return home the next day. They need to come for follow-up visits for the change of dressings and suture removal. Splints are continued after the surgery till the scars mature. Pressure garments are worn once the wounds have settled. They help in reducing the swelling and discomfort at the operated site. Patients can usually return to light work one week after the procedure. What are the measures taken during follow-up of burn scar surgery? In addition to the follow-up visits, patients are advised to use splints and pressure garments. Physical therapy is important for maintaining adequate range of motion and to keep the treated areas supple. Why are splints used? They help in resisting the contractile forces of a scar. During the early postoperative period, they are worn constantly. Later on, they are used during the night. What are the benefits of burn scar surgery? They help the person regain useful function of the affected part. This can mean the ability to earn and look after oneself. Burn scar surgery also improves the appearance of the affected part. They are associated with improvement in self-esteem and confidence. For more information on scars, visit here.
Scars are common and vary from mild to severe. They are the natural result of healing of injury which can be as a result of infection, trauma, burns or other causes. When scars are severe it can lead to cosmetic and functional problems. These, in turn, can cause psychological impairment of the affected individual. Even though it is impossible to completely eliminate scars, it is possible to improve them.
The various procedures for improvement of scars range from less invasive techniques to surgical correction. Each of these procedure has certain advantages and disadvantages compared to others. So a technique that may be effective in a certain type of scar may not have a similar benefit in another. It is seldom one approach suits all. Less invasive techniques include dermabrasion, peels, and LASERS. These are useful for mostly superficial scars. Superficial scars do not involve all the layers of skin. Type of scars amenable to surgical procedures Such type of scars would include the following 1. Deep scars 2. Contractures (scars with distortion of surrounding structures) Deep scars involve most of the layers of skin. In some cases, scars can draw attention due to their orientation across the natural skin creases (lines). Contractures occur due to the progressive contraction of scar tissue. Across mobile areas like joints, these contractures can limit the movement. For example, a burn contracture across the fingers can reduce the function of the hand. During surgical correction, these contractures are first removed and the resulting wound is covered with a graft or flap such that free movement is possible across the joints. Treatment options for surgical correction of scars The goal of plastic surgery would be an improvement in appearance and function. This is brought about by redistribution of tissues. The most commonly applied techniques include, Scar revision: During scar revision the scar is removed and neighboring tissues are brought together. Stretched out scars can be narrowed down with an approximation of dermis. A straight line scar can be broken down for a more pleasing outcome. In mild contractures, Z-plasty and Y-V plasty can be used for scar lengthening and functional relief. Most of these cases are carried out as outpatient procedures and patients can return home soon afterward. Serial excision: Sometimes it may not be possible to remove an entire scar and close the wound by approximation of the neighboring tissues. In such situations, it may be possible to remove the scar in stages. This is commonly adopted for removal of burn scars and naevi. Split thickness skin grafts: This is indicated when large areas need to be covered after a release of extensive contractures. Skin grafts are obtained from the top layers of skin and transferred for coverage of wounds. An advantage is the ability to cover large wounds in a single stage. The release of burn contractures and coverage with split thickness skin grafts result in a dramatic improvement of function. Skin grafts are usually obtained from lower extremity. The donor site heals by itself. Full thickness skin grafts: The full thickness of skin is used to cover the wounds following removal of the scar. These are cosmetically superior compared to split thickness skin grafts. Full-thickness grafts are limited by the limited availability. The donor site can usually be managed with straight line closure. Flaps: Flap surgery involves recruitment of neighboring or distant tissue with its blood supply for coverage of the wounds. They have the advantage of mobilization of tissues with similar texture and appearance. Tissue expanders: These are inflatable devices placed under the skin and adjacent to a scar. Once the operated site heals, these expanders are gradually inflated with saline. Over a period of time, this leads to stretching of the overlying skin. Once an adequate expansion is achieved the expanders are removed and the redundant skin is used to cover the wound after removal of the scar. Tissue expanders are useful in coverage of large areas with tissues similar to the native tissue. Timing to undergo plastic surgery for scar improvement It is advisable to undertake surgery once the scar has matured. This can take more than a year. During this time, the scar tends to become soft and supple. An exception to this would be cases with contractures causing significant impairment of function. For example, a scar of the neck which prevents the patient from carrying out daily activities needs early release and coverage. Patients should be in good health at the time of any elective surgery. Recovery following scar revision Most of the procedures are outpatient or short stay procedures. Depending upon the location and extent of the procedure, anesthesia can be local or general anesthesia. Patients need to follow up regularly after surgery. Use of silicone sheet, splints, and pressure garments form a part of the post-operative management. Benefits of undergoing surgical scar revision These would include, 1. Improvement in appearance and function. 2. Improved confidence and self-esteem. To learn more about scars, click here. |
AuthorI like to keep it simple. CategoriesArchives
June 2024
Categories |
- Home
-
Cosmetic
- Fat grafting
- Swellings and moles
- Scar revision
- Leukoderma (Melanocyte transfer)
- Hair transplant
- Facial rejuvenation procedures
- Nose job (Rhinoplasty)
- Cleft lip nose correction
- Ear (Otoplasty)
- Lip reduction
- Breast augmentation
- Breast reduction
- Tuberous breasts
- Axillary breasts
- Gynecomastia
- Liposuction
- Brachioplasty (Arm contouring)
- Abdominoplasty (Tummy tuck)
- Female genital rejuvenation
-
Reconstructive
- Contact
- Blog
- Home
-
Cosmetic
- Fat grafting
- Swellings and moles
- Scar revision
- Leukoderma (Melanocyte transfer)
- Hair transplant
- Facial rejuvenation procedures
- Nose job (Rhinoplasty)
- Cleft lip nose correction
- Ear (Otoplasty)
- Lip reduction
- Breast augmentation
- Breast reduction
- Tuberous breasts
- Axillary breasts
- Gynecomastia
- Liposuction
- Brachioplasty (Arm contouring)
- Abdominoplasty (Tummy tuck)
- Female genital rejuvenation
-
Reconstructive
- Contact
- Blog
You can leave us a comment using the contact form below.
We shall get back to you at the earliest.
We shall get back to you at the earliest.
Links
- Face procedures | Rhinoplasty, Otoplasty, Lip reduction, Fat grafting
- Body procedures | Gynecomastia , Breast reduction, Abdominoplasty, Brachioplasty, Liposuction
- Skin procedures | Scar revision, Moles, Leukoderma surgery
Let's be friends !
Follow us at Facebook and Twitter.
Follow us at Facebook and Twitter.
© 2024 Amicus Clinic (Plastic Surgery Centre, Trivandrum). All rights reserved.

 RSS Feed
RSS Feed



