|
Smoking and plastic surgery
Smoking is bad for plastic surgery. It can lead to complications and adversely affect the outcomes of a surgical procedure. This can be due to various reasons. Let me elaborate.
When to stop smoking before surgery? The best time to stop smoking is now. The negative effects of smoking reduce after cessation of smoking. We usually advise a period of 4 to 6 weeks of abstinence before undertaking any surgery. Plastic surgery can involve extensive dissection of the tissues. This makes healing more dependent on adequate blood supply of the treated tissues. Because of the above reasons, smoking is a strong contrindication for surgery. Smoking is also one of the common reasons for postponement of the surgery in our practice. We usually choose to schedule surgery after a period of abstinence from smoking. For further reading about the effect of smoking during surgery, please visit: https://www.who.int/news/item/20-01-2020-smoking-greatly-increases-risk-of-complications-after-surgery There is an increasing demand for cosmetic procedures with minimal downtime. The advantages are shorter recovery and the ability to return to normal life. One such procedure is non-surgical rhinoplasty.
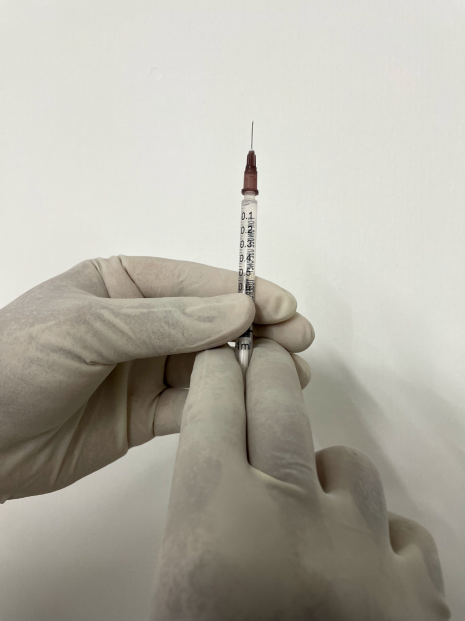
What is a non-surgical rhinoplasty? It involves the injection of fillers into the nose to bring about a difference in appearance. It has more in common with a filler injection into the face than with a routine rhinoplasty. The 'rhinoplasty' in non-surgical rhinoplasty comes because the filler is being injected into the nose to alter its appearance. Non-surgical rhinoplasty is also referred to as liquid rhinoplasty. Why 'liquid'? Because the filler that is injected is a liquid. What are the advantages of doing a non-surgical rhinoplasty? The main advantage of such a procedure would be the minimal downtime. Since fillers are injected the time taken to complete the procedure would be very short and would not need any hospital admission. What can be achieved with non-surgical rhinoplasty? Compared to a surgical procedure, the benefits of a non-surgical procedure are limited. The benefits of a non-surgical rhinoplasty include,
What are the changes that can't be achieved with rhinoplasty? It is not possible to make a large nose smaller using injection non-surgical techniques. It is also not useful for the management of a bulbous tip. It is not possible to improve septal deviations with non-surgical rhinoplasty. Surgical rhinoplasty is the gold standard for the management of the deformities of the nose. How long does the effect of non-surgical rhinoplasty last? When compared to a surgical procedure, the effects of non-surgical rhinoplasty are temporary. In most cases, hyaluronic acid fillers are injected during this procedure. Hyaluronic acid breakdown with time. The effects may last approximately one to two years. In certain individuals, the effects tend to last for a shorter period. In case of an unfavourable result, it can be removed with the help of a hyaluronidase injection. What are the risks associated with non-surgical rhinoplasty? The risks associated with a non-surgical rhinoplasty are similar to those seen with filler injections into the face. These can include tissue death and involvement of the vessels of the eyes and brain. Skin necrosis results due to impaired blood supply of the skin. Embolization of the filler into the vessels of the eyes can lead to blindness. These adverse events have been reported with filler injections, they are uncommon. Who is a good candidate for non-surgical rhinoplasty? It would include patients who want a change in the appearance of the nose without any downtime or need for aftercare associated with a conventional rhinoplasty. Patients should have realistic expectations and understand that not all deformities can be improved with a non-surgical rhinoplasty. The effects are temporary and need repeat injections for maintenance of the results. For more information about rhinoplasty please visit: www.amicusclinic.in/rhinoplasty Rhinoplasty is a commonly known plastic surgery procedure to improve the appearance and function of the nose. The function of the nose relates to breathing. As in all surgical procedures, complications can happen. The goal of preoperative evaluation is also to seek out any potential problem. But despite the best efforts, complications can occur.
The incidence of the complications varies. It can vary depending on the type of procedure, and patient factors. It is more common to have a greater incidence of complications in difficult (challenging) cases. Some of the complications are uncommon when compared to others. The complications can be seen under those that are nonspecific to rhinoplasty and those specific to rhinoplasty. The nonspecific complications can occur in any surgical procedure. It need not be in rhinoplasty alone. These include,
The specific complications of rhinoplasty are those related to aesthetic (appearance) and functional (breathing). The aesthetic complications include,
Functional problems associated with rhinoplasty include,
Some of the complications are more serious when compared to others. Also, the difficulty level in performing a rhinoplasty can vary depending on the presentation. It is also more so in previously operated noses. It is not possible to eliminate the possibility of complications. However, it is usually possible to reduce their incidence with careful planning and attention to detail. For more details about rhinoplasty, visit here. Pushback otoplasty is done for improvement in the appearance of prominent ears. It is usually carried out under general anesthesia in children and local anesthesia in adults. During this procedure, ear cartilage is removed and reshaped so that it lies closer to the head. It is carried out either as a short stay or outpatient procedure. Pain is controlled with the help of oral medications.
After the procedure, a dressing is given in the form of a head wrap with a bandage. The ears are inspected on the first postoperative day for the presence of any collection. The bandages are retained for a week. At the end of the week, the dressings are removed. Patients can shower once the dressings are out. For two weeks following the procedure, a headband is advised to be worn constantly. After this period, a headband should be worn during the night. It is common to have swelling of ears following surgery. This gradually subsides over time. Most of the swelling disappears by the end of a month. Pushback otoplasty is a cosmetic procedure. It does not alter the hearing. It helps individuals with prominent ears to obtain a better body image. Click here, for more information on otoplasty. Earlobe repair is a commonly requested procedure in our practice. A wide aperture results in an ungainly appearance with dangling of disc-shaped earrings. There is also a risk of complete disruption of the bridge of tissue and a split earlobe.
Earlobe repair is done under local anesthesia as an outpatient procedure. We usually perform our repair using a technique that helps us to avoid a further session of ear piercing. The existing hole is modified such that it becomes smaller and retains its original position. This avoids the risk of having an eccentric position of the aperture during a secondary piercing. Individuals who come for earlobe repair should have an understanding of the reasons for the deformity. Heavy earrings and multiple trivial trauma lead to a lengthened aperture. It is prudent to avoid heavy earrings after a repair. The repair has an approximate strength of ten percent of the intact neighboring skin. This increases to fifty at three months and seventy at one year. This is independent of the technique and is related to our wound healing and scar strength. And because of this, we advise our patients to avoid heavy earrings for one year following a repair. This helps contribute to the longevity of a good result. Hello, is this the plastic surgery clinic? Yes. Do you perform rhinoplasty? Yes, we do. What is the cost of rhinoplasty? We need to see you before we comment on the treatment plan or the cost. Is it possible to give a rough estimate? ……. We tend to have the above conversation multiple times. Sometimes rhinoplasty gets replaced by another procedure such as liposuction, fat grafting or something else. I thought of elaborating more about our resistance to comment on treatment costs before seeing the patient. Imagine a person with a desire to build a home. Not an apartment in a high-rise, but someplace on a piece of land with a small garden. Such a person would have certain ideas about size, location, immediate vicinity, style, etc. And if there is a lack of clarity related to these aspects she would assume that she would be guided by an expert. Now let's imagine another conversation. Hello, is this the builder's office? Yes. Do you build homes? Yes, we do. What is the cost of building a home? …….. We find both these conversations very similar. Because we are dealing with situations in which making plans would not make sense without a good grasp of what the customer needs. In other words, both cosmetic surgery and building a home are highly customized endeavors. There are a lot of variables which need to be sorted out or understood before we finalize a plan. In both cases, the expert brings to the table his or her expertise. Once a plan is finalized it is reasonable to arrive at the cost. It is nearly impossible to follow a cookie cutter approach in cosmetic surgery. Let me give an example. Let us assume an individual seeking rhinoplasty. Following a clinical examination and discussion, we usually arrive at a treatment plan. A plan found suitable for one person may be quite different from a plan for another individual. One may require a short procedure lasting one hour whereas the other may require something much more complex lasting six hours. The cost, in turn, depends on the complexity and duration of a treatment procedure. Like an architect who seeks input from her client, we give a lot of importance to input from our patients. This more so in cosmetic surgery when compared to other surgical specialties. Because of this, a similar looking deformity may get treated using different techniques. One individual may be satisfied with a simple correction whereas another may be keen on a more exacting remedy. This again reflects on the cost of the procedure. This sort of variability in treatment options applies to almost procedures in cosmetic surgery. Because of these reasons we hesitate to comment on any treatment plan when certain pictures or images are sent to us. We do get an approximate idea of the deformity with the images, but in the absence of a discussion with the patient, it does not make much sense to decide on a treatment plan. Also, a clinical examination gives a lot of important and useful information relating to the management of the condition. These are not otherwise apparent by inspecting images of the body part. To give an example, in rhinoplasty we get to assess aspects like the thickness of the skin and soft tissue, structural support, status of the nasal cavity as well as nasal obstruction with a clinical examination. These can't be inferred from the pictures. It may sometimes be possible to give an estimate of the cost when a procedure is simple or straightforward. This applies to procedures like excision of a mole with a straight-line closure or repair of an earlobe cleft. This can also apply to procedures like hair transplant when the cost can be correlated in terms of a smaller unit say, cost per follicular unit. All of the above reasons lead to a reluctance to comment on the cost of a procedure without a clinical examination and discussion. I suppose similar reasons would also apply to those who seek to get a home built somewhere.
Deep wrinkles of the forehead are commonly seen in an aging face. They are usually seen in the area between the eyebrows. They tend to give a serious look to the affected individual. In the beginning, these wrinkles become apparent during facial expressions. Later on, they become fixed and are constantly present. Lowering of the eyebrows can be associated with the appearance of these wrinkles.
Because of their position, these wrinkles are immediately apparent to an onlooker. The wrinkles are as a result of the contraction of underlying muscles of the forehead. The skin becomes thin with age and as a result of the contraction of the underlying muscles, the overlying tissues gets folded in like an accordion. These wrinkles can be improved by both nonsurgical and surgical techniques. Nonsurgical treatments: This is comprised of injections with botulinum toxin and dermal fillers. The nonsurgical procedures are preferred by many as these are performed as outpatient procedures. They do not have a downtime and patients can get back to their routines soon after the procedure. 1. Botulinum toxin injection: Botulinum toxin acts on the junction between the nerves and muscles to prevent transmission of impulses. This causes relaxation of the forehead muscles which are responsible for wrinkles. A small needle is used to inject to treat the targeted muscles. The full effect of the injections takes approximately one week. The effect lasts for around six months. For continuing action, these injections need to be repeated once the effect wears off. 2. Filler injections: As the name suggests they 'fill up' areas. As we age we undergo volume loss of the soft tissues. This includes the skin and deeper tissues of the face. Fillers counteract these changes by addition of volume. There are various fillers which differ based on their constituent molecule, and duration of action. The most commonly used fillers are made of hyaluronic acid. They are injected into the skin with the help of fine needles. They soften the wrinkles by making the skin firmer. Filler injections can also be used at a deeper level adjacent to the bones. Deep and static wrinkles of the forehead usually need treatment with a combination of fillers and botulinum toxin injections. Surgical treatment: Unlike nonsurgical treatments, surgical therapy is more invasive. A brow lift is a technique used for surgical rejuvenation of the forehead. Brow lift: A brow lift is also known as a forehead lift. It addresses age-related changes such as: 1. the wrinkles of the forehead, 2. the wrinkles between the eyebrows, 3. the lowering of the eyebrows. It results in a higher resting position of the eyebrows and, 4. improves the hooding of the eyelids as a result of the lower position of the eyebrows. A good candidate for a brow lift would be one who is in good health, has reasonable expectations about the procedure and is a non-smoker. A brow lift is performed under general anesthesia. The incision is placed usually behind the hairline. The tissues of the forehead are elevated to a higher position and excess skin is trimmed away. Brow lift requires an overnight stay in the hospital. A drain may be placed temporarily to prevent collection at the operated site. The sutures are removed at ten days. Patients can return to work at the end of a week. Most of the swelling following brow lift abate by the end of one month. The results of the brow lift, though invasive last much longer than the office-based procedures. Deep wrinkles of the forehead can be managed effectively both by means of simple office based procedures and a surgical brow lift. They vary in their indications, downtime, and permanency of results. As in all injuries, burns end up as scars. The deeper burns usually give rise to problem scars. These scars can be a cause of disability and impair quality of life of the affected individual. It can lead to problems relating to self-esteem. However, it is possible to improve these scars with the help of restorative surgery. This forms one of the most rewarding specialties of plastic surgery. Restoration means an improvement of both the form and function of the affected part. How do burn scars lead to impairment of function? Scars differ from the native tissue it replaces. They are less elastic and tend to contract with time. Due to this intrinsic property of contraction, scars reduce the movement of structures associated with it. For example, scars stretching across the front (anterior surface) of the elbow can reduce the ability to straighten out the elbow. This leads to a reduction in function of the affected upper limb. In a manual laborer, this can mean the loss of ability to earn his/her livelihood. Scars also look and feel different compared to the unaffected (native) skin. This causes disfigurement. Deformity due to scars can make an individual shun social encounters. What are the indications for surgery for burn scars? They mainly done for two reasons: 1. Functional: When the scar impairs the function of the affected part. Burns affecting the hand may prevent the individual from using the part. With surgical treatment, it is possible to regain useful function of the hand. 2. Cosmetic: Scars can result in deformities. It is usually possible to surgically modify them and improve their appearance. Who are good candidates for burn scar surgery? Good candidates include those who are in good health and have reasonable expectations about the corrective surgery. When does one undergo surgical correction of burn scars? Scars are living tissues which undergo change in a appearance and texture with time. This is sometimes referred to as maturation of a scar. This can around eighteen months and surgery for scars are undertaken once the scars mature. However, in certain instances when the scars are associated with severe functional problems they are corrected earlier. For example, the involvement of the eyelids with scars can result in an absence of eyelid closure. This can lead to ulceration of cornea and blindness. In such a situation scars are treated without waiting for the scars to mature. What are the techniques used in scar surgery? Generally, the scars are cut and the resulting defect (gap) is covered either with neighboring tissues (local flaps) or skin grafts. The exact technique chosen depends on the deformity, treatment options and aesthetic and reconstructive goals of the patient. It is often possible to treat a deformity by more than one technique. Some of the procedures include: Skin grafts: These involve the transfer of the outer layers of the skin to cover a wound elsewhere. The area from where the grafts are obtained heal by itself. Grafts are an attractive option since they are abundantly available. Skin grafts tend to undergo contraction in the postoperative period. Because of this use of splints and pressure garments are important during the postoperative period. Flaps: They are tissues with the associated blood vessels transferred for coverage of a defect. They provide thicker tissues compared to skin grafts. Flaps closely mimic the native tissue in appearance and texture. Thus, they are usually aesthetically superior when compared to skin grafts. Flaps do not contract like skin grafts and once the wounds heal they are easier to manage and do not require rigorous use of splints. Tissue expanders: These are devices which are placed surgically underneath the skin adjacent to a scarred area. During the follow-up visits, they are progressively filled with saline. The inflation of the expanders causes the overlying tissues including skin to get stretched. Once a critical volume is achieved the expanders are removed and the extra skin is used to cover the scarred area. The advantage of such a procedure is that they provide tissues which bear a close resemblance to the native (original) tissue. They are frequently used to treat scars of the scalp. The use of adjacent scalp tissue enables the scar the be replaced with hair-bearing skin. Serial excision: Due to the size of a scar it may not be possible to close the wound edges after removal of the scar. During serial excision, this process is done in stages when a part of the scar is removed during each step. This takes advantage of the increased laxity of the tissues as they respond to the increased tension at the operated site. The advantage of serial excision is that they help narrow a broad scar without the use of additional grafts or flaps. What type of anesthesia is used for burn surgery? Surgery for burn scars is done under local or general anesthesia. General anesthesia is used in children and in adults when the area being treated is extensive. Local anesthesia is used in adults when the area affected is small. What is the recovery following a burn scar surgery? Burn scar surgery is usually performed as a short stay procedure. Patients can return home the next day. They need to come for follow-up visits for the change of dressings and suture removal. Splints are continued after the surgery till the scars mature. Pressure garments are worn once the wounds have settled. They help in reducing the swelling and discomfort at the operated site. Patients can usually return to light work one week after the procedure. What are the measures taken during follow-up of burn scar surgery? In addition to the follow-up visits, patients are advised to use splints and pressure garments. Physical therapy is important for maintaining adequate range of motion and to keep the treated areas supple. Why are splints used? They help in resisting the contractile forces of a scar. During the early postoperative period, they are worn constantly. Later on, they are used during the night. What are the benefits of burn scar surgery? They help the person regain useful function of the affected part. This can mean the ability to earn and look after oneself. Burn scar surgery also improves the appearance of the affected part. They are associated with improvement in self-esteem and confidence. For more information on scars, visit here. Fat grafting is a technique wherein living fat cells are transferred from one part of the body to another. The transferred cells obtain blood supply from its new location. Since they become integrated with the body they tend to be last long. This is in contrast to the injectable fillers which produce temporary results and need to be repeated at intervals for volume enhancement. What are the benefits of fat grafting? Fat grafting provides an increase in soft tissue volume. This helps in obtaining a more youthful proportion. Aging changes of face and body are associated with laxity (loose) of skin with loss of the volume of the underlying tissues. These changes are partially reversed with fat grafting. What are the areas which can be treated with fat grafting? Fat grafting techniques are used for improvement of 1. Face: Cheeks, Forehead 2. Breasts 3. Buttocks (Brazilian butt lift) 4. Scars ( Depressed scars) Where is the fat harvested from? Abdomen and thighs are the sites commonly used as donor areas for fat harvesting. This has the added benefit of improving the contours of these areas. Who is a right candidate for fat grafting? This would include individuals who need volume enhancement but want to avoid the use of any artificial substances. The volume enhancement in the case of breast augmentation with fat transfer would be lesser when compared to the conventional silicone implants. Individuals for fat grafting should have good health and not have any serious comorbid illness. It is also important to have realistic expectations about the outcomes which can be achieved with the procedure. How is fat transfer performed? It begins with a consultation when a surgeon evaluates you to find out if you are a right candidate for the procedure. A treatment plan is made which depends on the physical features as well as the treatment expectations of the individual. Fat grafting to face may involve multiple sessions wherein small quantities are transferred to avoid over correction. Anesthesia for the procedure is either with local or general anesthesia. This depends on the extent and areas being treated. Fat grafting to areas in the face is done under local anesthesia. Breast and buttocks are treated under general anesthesia. Fat is harvested from the thighs and abdomen with thin cannulas. The harvested tissues are processed to increase the fraction of viable cells which would then be transferred back into the body. The processed tissue is injected back into the recipient sites with thin cannulas. Patients can soon return home after correction of smaller areas. More extensive grafting though performed as a short stay or day care procedure and individuals can return to work in a week. Recovery from fat grafting will include swelling at the treated site. This is more prominent at highly vascular sites like face. This gradually subsides with time and usually does not need any specific treatment. What are the possible complications of the procedure? The complications specific to fat grafting will include: 1. Fat did not last long enough: This can be lessened with refinements of harvesting and processing the fat. Fat transfer does suffer from a lack of precise predictability of the take. It tends to take up better in highly vascular areas like the face. It tends to be lost more in highly mobile areas like lips. 2. Over grafted look: This can be avoided by carrying out the procedure in small sessions and trying to avoid over correction. This complication probably results from the treating doctor trying to compensate for the possible loss of the fat cells with time. 3. Irregular and lumpy appearance: This is seen in areas where the overlying skin is very thin. This can be minimized with grafting at deeper planes. What are the benefits of volume augmentation with fat grafting? Since we are using part of the body for volume enhancement, it tends to 1. Last a long time when integrated by the body (this is in contrast to the temporary fillers). 2. Do not suffer from extrusion as can happen with foreign implants.
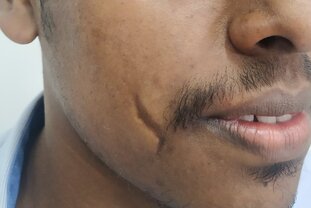
Scars are common and vary from mild to severe. They are the natural result of healing of injury which can be as a result of infection, trauma, burns or other causes. When scars are severe it can lead to cosmetic and functional problems. These, in turn, can cause psychological impairment of the affected individual. Even though it is impossible to completely eliminate scars, it is possible to improve them.
The various procedures for improvement of scars range from less invasive techniques to surgical correction. Each of these procedure has certain advantages and disadvantages compared to others. So a technique that may be effective in a certain type of scar may not have a similar benefit in another. It is seldom one approach suits all. Less invasive techniques include dermabrasion, peels, and LASERS. These are useful for mostly superficial scars. Superficial scars do not involve all the layers of skin. Type of scars amenable to surgical procedures Such type of scars would include the following 1. Deep scars 2. Contractures (scars with distortion of surrounding structures) Deep scars involve most of the layers of skin. In some cases, scars can draw attention due to their orientation across the natural skin creases (lines). Contractures occur due to the progressive contraction of scar tissue. Across mobile areas like joints, these contractures can limit the movement. For example, a burn contracture across the fingers can reduce the function of the hand. During surgical correction, these contractures are first removed and the resulting wound is covered with a graft or flap such that free movement is possible across the joints. Treatment options for surgical correction of scars The goal of plastic surgery would be an improvement in appearance and function. This is brought about by redistribution of tissues. The most commonly applied techniques include, Scar revision: During scar revision the scar is removed and neighboring tissues are brought together. Stretched out scars can be narrowed down with an approximation of dermis. A straight line scar can be broken down for a more pleasing outcome. In mild contractures, Z-plasty and Y-V plasty can be used for scar lengthening and functional relief. Most of these cases are carried out as outpatient procedures and patients can return home soon afterward. Serial excision: Sometimes it may not be possible to remove an entire scar and close the wound by approximation of the neighboring tissues. In such situations, it may be possible to remove the scar in stages. This is commonly adopted for removal of burn scars and naevi. Split thickness skin grafts: This is indicated when large areas need to be covered after a release of extensive contractures. Skin grafts are obtained from the top layers of skin and transferred for coverage of wounds. An advantage is the ability to cover large wounds in a single stage. The release of burn contractures and coverage with split thickness skin grafts result in a dramatic improvement of function. Skin grafts are usually obtained from lower extremity. The donor site heals by itself. Full thickness skin grafts: The full thickness of skin is used to cover the wounds following removal of the scar. These are cosmetically superior compared to split thickness skin grafts. Full-thickness grafts are limited by the limited availability. The donor site can usually be managed with straight line closure. Flaps: Flap surgery involves recruitment of neighboring or distant tissue with its blood supply for coverage of the wounds. They have the advantage of mobilization of tissues with similar texture and appearance. Tissue expanders: These are inflatable devices placed under the skin and adjacent to a scar. Once the operated site heals, these expanders are gradually inflated with saline. Over a period of time, this leads to stretching of the overlying skin. Once an adequate expansion is achieved the expanders are removed and the redundant skin is used to cover the wound after removal of the scar. Tissue expanders are useful in coverage of large areas with tissues similar to the native tissue. Timing to undergo plastic surgery for scar improvement It is advisable to undertake surgery once the scar has matured. This can take more than a year. During this time, the scar tends to become soft and supple. An exception to this would be cases with contractures causing significant impairment of function. For example, a scar of the neck which prevents the patient from carrying out daily activities needs early release and coverage. Patients should be in good health at the time of any elective surgery. Recovery following scar revision Most of the procedures are outpatient or short stay procedures. Depending upon the location and extent of the procedure, anesthesia can be local or general anesthesia. Patients need to follow up regularly after surgery. Use of silicone sheet, splints, and pressure garments form a part of the post-operative management. Benefits of undergoing surgical scar revision These would include, 1. Improvement in appearance and function. 2. Improved confidence and self-esteem. To learn more about scars, click here. |
AuthorI like to keep it simple. CategoriesArchives
June 2024
Categories |
- Home
-
Cosmetic
- Fat grafting
- Swellings and moles
- Scar revision
- Leukoderma (Melanocyte transfer)
- Hair transplant
- Facial rejuvenation procedures
- Nose job (Rhinoplasty)
- Cleft lip nose correction
- Ear (Otoplasty)
- Lip reduction
- Breast augmentation
- Breast reduction
- Tuberous breasts
- Axillary breasts
- Gynecomastia
- Liposuction
- Brachioplasty (Arm contouring)
- Abdominoplasty (Tummy tuck)
- Female genital rejuvenation
-
Reconstructive
- Contact
- Blog
- Home
-
Cosmetic
- Fat grafting
- Swellings and moles
- Scar revision
- Leukoderma (Melanocyte transfer)
- Hair transplant
- Facial rejuvenation procedures
- Nose job (Rhinoplasty)
- Cleft lip nose correction
- Ear (Otoplasty)
- Lip reduction
- Breast augmentation
- Breast reduction
- Tuberous breasts
- Axillary breasts
- Gynecomastia
- Liposuction
- Brachioplasty (Arm contouring)
- Abdominoplasty (Tummy tuck)
- Female genital rejuvenation
-
Reconstructive
- Contact
- Blog
You can leave us a comment using the contact form below.
We shall get back to you at the earliest.
We shall get back to you at the earliest.
Links
- Face procedures | Rhinoplasty, Otoplasty, Lip reduction, Fat grafting
- Body procedures | Gynecomastia , Breast reduction, Abdominoplasty, Brachioplasty, Liposuction
- Skin procedures | Scar revision, Moles, Leukoderma surgery
Let's be friends !
Follow us at Facebook and Twitter.
Follow us at Facebook and Twitter.
© 2024 Amicus Clinic (Plastic Surgery Centre, Trivandrum). All rights reserved.


 RSS Feed
RSS Feed



